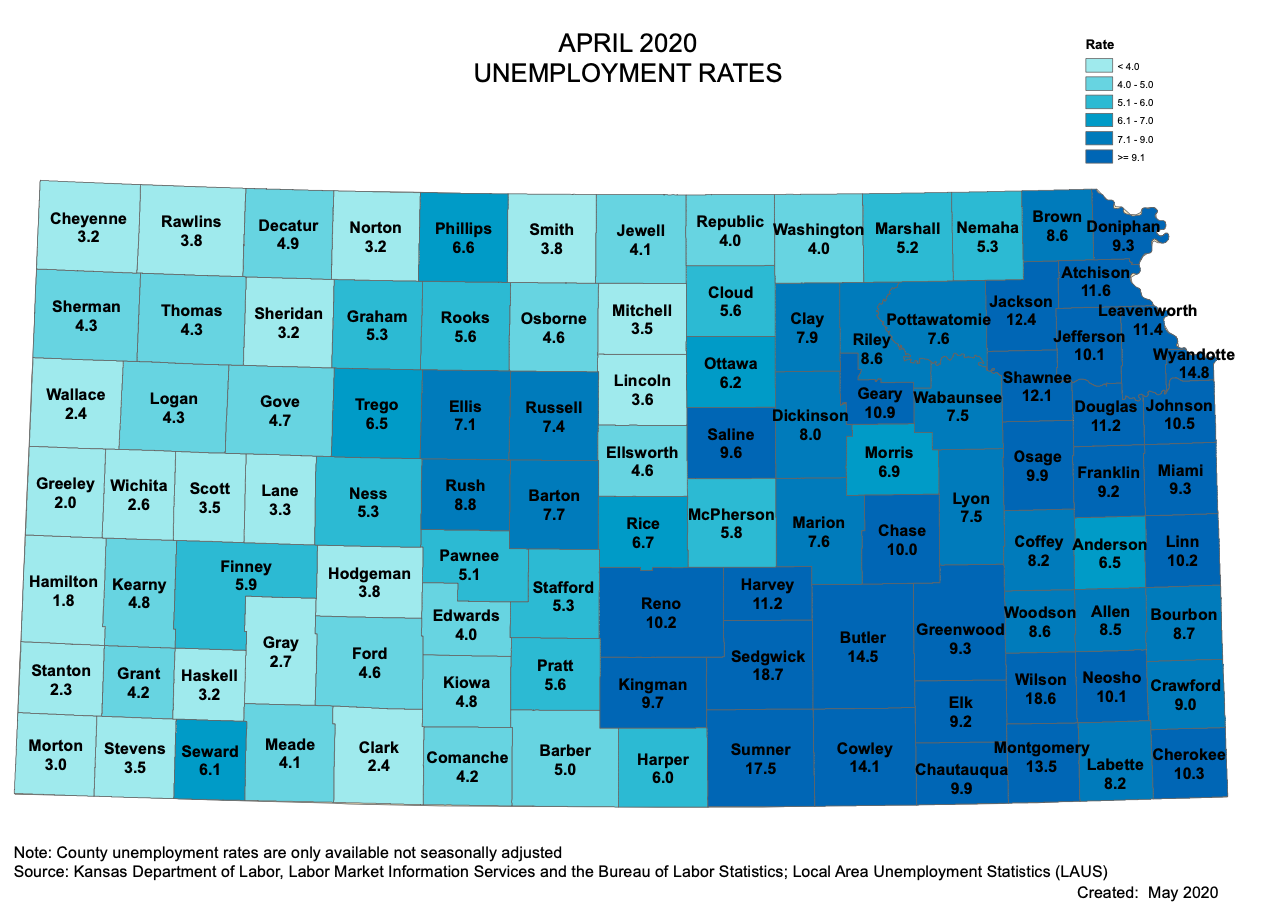
MISSION, Kan. (AP) — Kansas took a major step toward reopening Friday amid the coronavirus pandemic as unemployment numbers soared and a nursing home outbreak grew.
The seasonally adjusted unemployment rate hit 11.2% in April, an increase from a historical low of 2.8% in March, according to preliminary estimates from the Kansas Department of Labor. The U.S. unemployment rate is at 14.7%.
Seasonally adjusted job estimates indicate total Kansas nonfarm jobs decreased by 130,400 from March. Private sector jobs, a subset of total nonfarm jobs, decreased by 121,600 from the previous month, while government decreased by 8,800 jobs.
Emilie Doerksen, a labor economist for the state, said in a written statement that the estimates “reflect the impact of efforts to contain the coronavirus pandemic” and that “the leisure and hospitality sector saw a particularly sharp decline, accounting for 50,200 out of the total decrease since March.”
As Memorial Day weekend approached, the maximum size of mass gatherings increased from 10 to 15 people. State-owned casinos also were allowed to reopen, along with theaters, museums, bowling alleys and other indoor leisure places. But bars, nightclubs and swimming pools must stay closed for now.
Kansas Department of Health and Environment Secretary Lee Norman said Friday that it was crucial to “exercise caution and remain vigilant,” noting that “just because we are going into a new phase of reopening, the virus hasn’t gone away.”
The number of cases in the state rose by 419 cases Friday to 8,958, with 46% of the new cases in three southwest Kansas counties with meatpacking plants — Ford, Finney and Seward counties. Combined they have 3,740 cases, up 194 from Wednesday, the last day the state reported data. State health officials also reported 185 deaths, with seven deaths tied to outbreaks in the packing plants.



